Table of Contents
We know at this point, some of you might be already very familiar with Polycystic Ovary Syndrome or known as PCOS. PCOS is a hormonal disorder that affects women of reproductive age. It is characterized by irregular periods, high levels of androgen hormones, and the presence of cysts on the ovaries. Insulin resistance, a condition in which the body becomes less sensitive to insulin, is also commonly associated with PCOS. Now let’s explore the link between PCOS and insulin and how it affects PCOS girlies out there!
Insulin Resistance in PCOS

Insulin or blood sugar hormone is a hormone produced by the pancreas that regulates blood sugar levels in the body. Insulin resistance occurs when the body becomes less responsive to insulin, leading to high blood sugar levels. This can lead to the development of type 2 diabetes if left untreated. Insulin resistance is a common feature of PCOS, affecting up to 70% of women with the condition.
The exact cause of insulin resistance in PCOS is not fully understood. However, it is thought to be linked to the high levels of androgen hormones, such as testosterone, which are often present in women with PCOS. These hormones can interfere with the action of insulin, making the body less responsive to its effects.
Insulin resistance can also lead to the production of more androgen hormones, creating a vicious cycle that can exacerbate the symptoms of PCOS. High insulin levels can also lead to weight gain, which is another risk factor for PCOS.
Impact of Insulin Resistance on PCOS Symptoms
 Insulin resistance can worsen the symptoms of PCOS, making it more difficult to manage. One of the most common symptoms of PCOS is irregular periods, which can be caused by high levels of androgen hormones. Insulin resistance can further disrupt the menstrual cycle by affecting the production of other hormones, such as luteinizing hormone (LH) and follicle-stimulating hormone (FSH). This can lead to a lack of ovulation and infertility.
Insulin resistance can worsen the symptoms of PCOS, making it more difficult to manage. One of the most common symptoms of PCOS is irregular periods, which can be caused by high levels of androgen hormones. Insulin resistance can further disrupt the menstrual cycle by affecting the production of other hormones, such as luteinizing hormone (LH) and follicle-stimulating hormone (FSH). This can lead to a lack of ovulation and infertility.
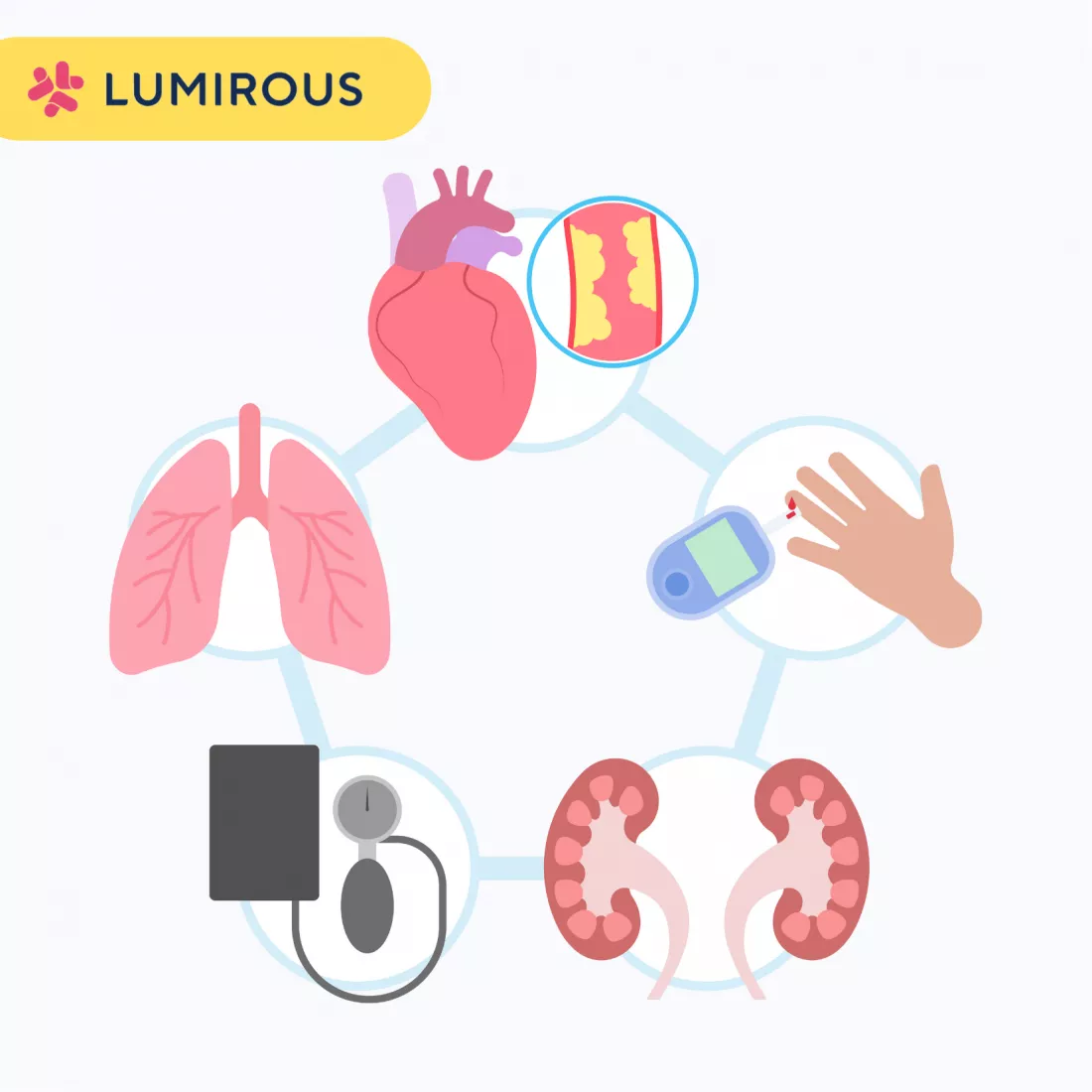 Insulin resistance can also increase the risk of developing other health conditions, such as type 2 diabetes, high blood pressure, and heart disease. Women with PCOS are already at an increased risk of these conditions, so insulin resistance can compound this risk.
Insulin resistance can also increase the risk of developing other health conditions, such as type 2 diabetes, high blood pressure, and heart disease. Women with PCOS are already at an increased risk of these conditions, so insulin resistance can compound this risk.
Treatment Options
 There are several treatment options available for women with PCOS and insulin resistance. The primary goal of treatment is to reduce insulin levels and improve insulin sensitivity. This can be achieved through lifestyle changes, such as taking the right food and supplements and low-impact exercises such as yoga. Weight loss can also improve insulin sensitivity and reduce the symptoms of PCOS.
There are several treatment options available for women with PCOS and insulin resistance. The primary goal of treatment is to reduce insulin levels and improve insulin sensitivity. This can be achieved through lifestyle changes, such as taking the right food and supplements and low-impact exercises such as yoga. Weight loss can also improve insulin sensitivity and reduce the symptoms of PCOS.
 Medications and supplements can also be used to improve insulin sensitivity in women with PCOS. Metformin is a commonly prescribed medication that helps to lower insulin levels and improve insulin sensitivity. It is also effective in reducing the symptoms of PCOS, such as irregular periods and hirsutism (excessive hair growth)
Medications and supplements can also be used to improve insulin sensitivity in women with PCOS. Metformin is a commonly prescribed medication that helps to lower insulin levels and improve insulin sensitivity. It is also effective in reducing the symptoms of PCOS, such as irregular periods and hirsutism (excessive hair growth)
Other medications, such as clomiphene citrate and letrozole, can induce ovulation in women with PCOS who are trying to conceive. These medications work by regulating the production of LH and FSH hormones, which are important for ovulation.
Insulin resistance is a common feature of PCOS and can worsen the condition's symptoms. It is important for PCOS girlies to take note of the link between insulin and PCOS and to take steps to manage their insulin levels. This can be achieved through taking the right food and supplements, low-impact exercises, and medication when necessary. With proper management, women with PCOS can of course lead a fulfilling and healthier life!
Make sure to stick around for more tips on fertility and reproductive health over here at LUMIROUS.
